Continuous Glucose Monitoring Devices: What CGMs Can (and Can’t) Reveal About Metabolic Health
Continuous glucose monitoring devices (CGMs) are helpful tools for monitoring blood sugar. These tools can be very informative for identifying trends in blood sugar patterns, for example whether low blood sugar (hypoglycemia) overnight may be contributing to sleep issues. However, most people are using CGMs to micromanage carbohydrate intake rather than understand why glucose behaves the way it does.
Believe it or not, blood sugar challenges are often not a carb problem. Let’s discuss how to use CGMs effectively and explore the deeper drivers of blood sugar dysregulation for lasting metabolic support, beyond food swaps and simple mealtime hacks.
Why Blood Sugar Can Be High Despite a “Healthy” Diet and “Normal” Insulin
Insulin is a hormone made by your pancreas that moves glucose (sugar) out of your bloodstream and into cells, especially liver and muscle cells, where it can be used for energy or stored for later. The more insulin sensitive you are, the more efficiently this glucose hand-off occurs, leading to steadier energy levels and more stable blood sugar. When insulin signaling begins to falter, blood sugar swings, fatigue, and longer-term metabolic issues can start to appear.
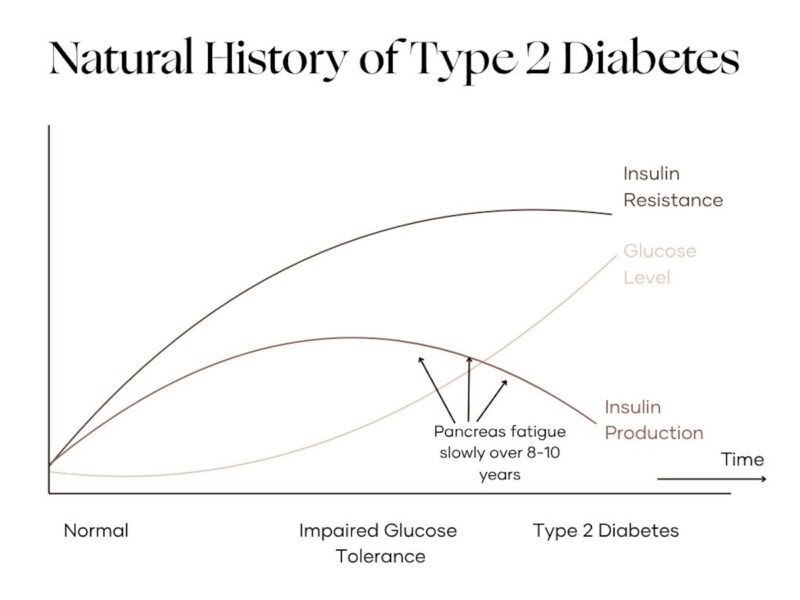
In the graph below, which depicts the natural progression of insulin resistance, you’ll notice that once glucose tolerance becomes significantly impaired, insulin levels begin to drop while glucose steadily rises. This entire process typically unfolds slowly, often over the course of 8-10 years.
This pattern can be confusing, especially if you eat a healthy diet and have been told your insulin is “normal.” If your fasting insulin falls within the optimal range (3-6 µIU/mL), yet your glucose levels still appear elevated on a CGM, it’s important to consider your broader metabolic context.
You don’t need a diagnosis of type 2 diabetes or prediabetes to see this pattern. It’s commonly observed in individuals who are highly active, chronically inflamed, hormonally imbalanced, or under-recovered or under-fueled from exercise. In other words, higher glucose readings do not automatically mean you are insulin resistant or eating “too many carbs.”
More specifically, elevated glucose with normal insulin often suggests:
- Impaired glucose uptake by the cells, meaning glucose isn’t efficiently moving into muscle and other tissues
- Cortisol (stress hormone) driven glucose release, particularly following low blood sugar levels
- Inflammatory interference at the cellular level, which disrupts insulin signaling even when insulin itself is adequate
Using CGMs the Right Way: It’s All About Trends, Not Absolutes
CGMs can be helpful tools, particularly for identifying trends and patterns within your blood glucose data. However, absolute values should always be interpreted with a degree of caution.
CGMs have a mean absolute relative difference (MARD) of approximately 8-14% compared to reference blood glucose measurements. Because CGM devices measure glucose in the interstitial fluid (the fluid surrounding your cells), shifts in blood sugar levels can appear delayed and less precise than direct blood glucose readings.
Research also shows that the younger and more metabolically stable the individual is, the less accurate CGM data tends to be when compared to blood glucose values. In contrast, CGM accuracy improves in individuals with insulin resistance or higher baseline glucose levels, as larger glucose fluctuations are easier for sensors to detect.
Rather than reacting to every spike, it’s more useful to focus on broader patterns, including:
- Post-meal glucose excursions – how high glucose rises and how quickly it returns to baseline. Ideally, balanced meals should cause no more than a 30-point glucose rise.
- Exercise-induced glucose elevations – which are often driven by a normal glucocorticoid (cortisol) stress response.
- Overnight glucose patterns – which can offer insight into stress levels, sleep quality, and liver glucose output.
- Other health factors – such as sleep deprivation, an activated immune system, or the luteal phase of the menstrual cycle, especially if these overlap with your CGM use.
Popular Blood Sugar “Hacks” vs. Reality
It’s helpful to have go-to tips and tricks to balance blood sugar more effectively around mealtimes, but the following common blood sugar hacks don’t always live up to the hype. We see this firsthand when analyzing our client’s CGM data. Let’s discuss where some of these tips may fall short.
Tip: Exercise After Meals
- Intensity matters more than timing!
- Low-intensity movement (especially zone 2 cardio) lowers glucose slowly and gradually.
- HIIT & strength training can spike glucose due to increasing cortisol production.
- Learn more in this episode of the Strength in Hormones Podcast.
Tip: Drink Apple Cider Vinegar Before Meals
- Benefits are mainly seen when consumed alongside complex carbohydrates (ex. beans, lentils, whole fruits, vegetables, quinoa).
- Minimal impact with simple carbs or mixed meals. Simple carbs include fruit juices, candy, most baked goods, and rice.
Tip: Swap for Gluten-Free Options
- Gluten-free does not mean lower carbohydrate.
- Many gluten-free alternatives are rice-based, which can cause similar or even higher glucose spikes than their non-gluten-free alternatives.
Tip: Eat Protein & Veggies First
- This is a great way to ensure that you’re eating adequate protein and antioxidants during your meals.
- However, fat intake may blunt glucose more effectively than protein alone. This is because fat intake slows digestion more significantly than protein or fiber, causing glucose from the carbs you eat to enter your bloodstream at a slower rate.
Tip: Get 10,000+ Steps Daily
- Research shows minimal additional benefits to blood sugar levels when walking more than 7000-7,500 steps per day, especially for women.
- More is not always better. Of course, this is highly dependent upon how you are moving throughout the day. Frequent short walks throughout the day can support blood sugar better than one long walk after sitting the entirety of the day.
Important reminder: If blood sugar is elevated, it doesn’t automatically mean carbs are the problem, or that insulin signaling is “broken.” Keep these insights in mind when considering daily strategies to help support blood sugar, but let’s unpack the real root of blood sugar dysregulation.
Why Balancing Blood Sugar Isn’t Just About Carb Intake
Blood sugar dysregulation and insulin resistance fall under the broader umbrella of metabolic dysfunction, which refers to impaired energy production and fuel utilization at the cellular level. Metabolic dysfunction is driven by far more than diet alone. To address it at the root, we must look at inflammation and immune signaling, mitochondrial health, and hormone regulation.
Inflammation & Immune Signaling
Chronic inflammation disrupts insulin signaling and glucose disposal, even when insulin levels appear “normal.” We emphasize “normal” because while optimal fasting insulin typically falls between 3–6 µIU/mL, many conventional lab reference ranges do not flag fasting insulin until levels exceed 18 µIU/mL. As a result, early blood sugar dysregulation can go undetected for years.
Mitochondrial Health
Glucose clearance and the conversion of carbohydrates into usable energy depend heavily on mitochondrial activity. When mitochondria are impaired, glucose remains in circulation instead of being efficiently converted into energy. This not only contributes to elevated blood glucose levels, but also creates an energy crisis or deficit at the cellular level, meaning your cells aren’t actually getting the fuel they need to function optimally.
Hormones That Matter Beyond Insulin
In addition to insulin, several hormones play critical roles in blood sugar regulation. Estradiol (E2), the predominant form of estrogen during the reproductive years, influences glucose transport in and out of cells and directly impacts insulin sensitivity. It does this by regulating GLUT4 expression, the primary glucose transporter in muscle and fat tissue.
T3 influences blood sugar regulation in multiple ways, from stimulating insulin release to regulating the liver’s ability to either break down stored glucose or produce new glucose. If you suspect low T3 may be contributing to your symptoms, you can explore this further in our free quiz.
Together, these hormonal shifts help explain why many women notice predictable CGM changes across the menstrual cycle, with blood sugar control often worsening during the late luteal phase.
Strategies to Actually Improve Blood Sugar Regulation Long-Term
Lasting blood sugar balance requires addressing the root drivers of metabolic dysfunction, rather than relying solely on quick mealtime tips and tricks. This means focusing on:
- Reducing chronic inflammation
- Restoring mitochondrial function
- Rebalancing hormones that govern glucose disposal (thyroid hormones, estradiol, cortisol)
- Supporting adequate exercise recovery, sleep, and nutrient sufficiency
Ultimately, blood sugar stability is a downstream marker of metabolic health. To meaningfully improve insulin sensitivity and glucose regulation, we must move beyond surface-level hacks and address what’s happening at the cellular and hormonal level.
Looking to Learn More?
CGMs are powerful when used to understand trends occurring in your body, not to punish food choices or see if you have “better scores than your friends.” When interpreted through the lens of inflammation, mitochondrial health, and hormones, they become tools for root-cause resolution.
As part of our 1:1 coaching program you receive exclusive access to our educational resources library. In it you’ll find our blood sugar deep-dive workshop, along with tons of other video resources. Learn more about our 1:1 program here, and book your free discovery call today!
Written by Romana Brennan, MS, RDN
Comments +